I allowed myself one week to keep eating as I had been, instead of jumping back into weight-loss mode right away. Figured it might be better on me both physically and mentally, being that my body was still pumped full of pregnancy hormones. This past week, though, I started purposefully increasing my activity level and tracking my food intake.
Monday: 30 min walk + PUSH DVD #2, Session #1
Tuesday: 30 min walk + 15 minutes of jogging on a trampoline (rebounding)
Wednesday: 30 min walk + PUSH DVD #2, Session #1
Thursday: 30 min walk + 10 minutes of DDR Supernova, workout mode (60 calories burned)
Friday: 30 min walk
I signed up for an account on SparkPeople, mainly because a.) I’d been tracking my food intake on their BabyFit website, and b.) I had previously been tracking my food using Diet Organizer on my PDA, but my PDA battery had died. I only recently replaced said battery, after I already got in the SparkPeople habit.
I’m planning to give my impressions of SparkPeople on an upcoming podcast, but I’ll mention here that I like it overall. It touts the “Spark Diet,” which is mainly just Eat Right And Exercise, but it’s really the tracking that does it. Plus, there are “trophies” members can achieve by earning SparkPoints online. SparkPoints can be had by entering food eaten, entering exercises done, tracking goals, reading articles, reading e-mails, logging in, and basically just surfing around the site. It’s an ingenious idea to generate return traffic, and to keep people entering their info daily.
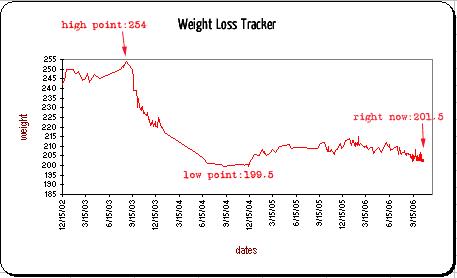
My weight hasn’t changed this week; I’m still at 201.5 lbs. I’m OK with that, though — at least I’ve lost and kept off the few pounds I put on in those two months of pregnancy. Now I have the chance to lose at least ten more pounds before we try again. The healthier I am, the better… although going through the medical game of 20 Questions at the hospital last month made me realize that my only major health issue IS my weight. Apart from that, I’m good to go. No heart disease, allergies, high blood pressure, any of that. So, count me lucky, I suppose.
Next week, I plan to measure myself and compare to my last measurements from September (if I can find them… I think I inadvertently threw away the sheet I’d recorded them on, thinking they were also in my PDA).
Here we go, on another fun weight-loss adventure. The way I figure, I should be able to jump in where I left off in the Fall, and keep on losing half a pound a week, if not more. If I can do that, I can lose ten pounds by the time we leave for our trip to Japan (during which I may end up gaining it all back). 🙂